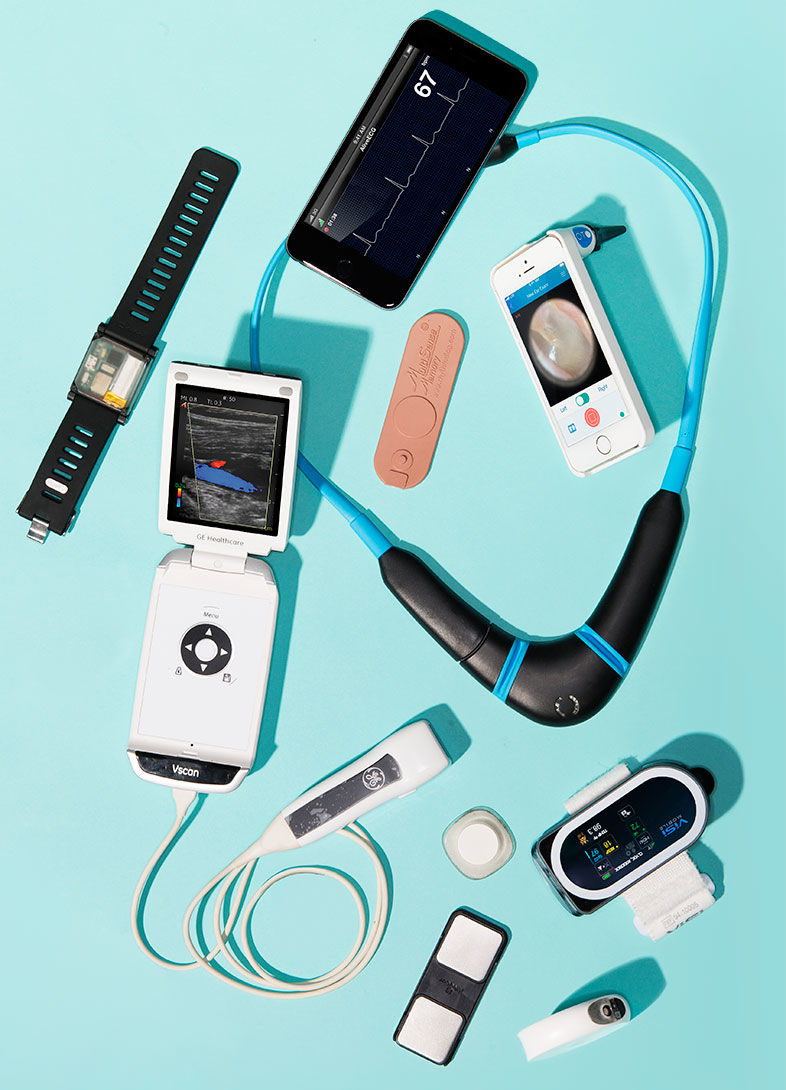
Healthcare Goes High-Tech
Photo by Robert Benson
Eric Topol is not satisfied with the health care status quo. The practicing cardiologist and director of the Scripps Translational Science Institute has seen the future of medicine and, in his view, we’re not getting there fast enough.
“We all recognize that the world has gone wireless,” Topol says. “Before we know it, 80 percent of adults will have a smartphone with broadband access. This digital infrastructure is moving at warp speed, but medicine basically hasn’t gotten out of the parking lot.”
Topol has a collection of smartphone-enabled devices that can measure vital signs and very nearly perform an entire physical. He’s used this gear to help distressed airline passengers in midflight, but he doesn’t want these tools to stay closed up in his (or any physician’s) black bag. He wants everyone to have access.
For more than 20 years, Topol has advocated for individualized therapies, genomic medicine, and digital tools, and it looks like policymakers are beginning to catch up. President Obama’s Precision Medicine Initiative seeks to leverage genomics to develop more effective treatments. Medicare is now reimbursing physicians for remote care, which can be provided through digital devices.
But Topol’s goals are far more ambitious. He wants to overturn the paternalistic relationship between physicians and patients. He envisions a more collaborative model, in which patients can have complete access to their medical data and partner with physicians on their care.
“Eric Topol is pushing the envelope by portraying a future that many patients, and especially many physicians, aren’t really ready for,” says Francis Collins, director of the National Institutes of Health. “While many of the things he has talked and written about are not yet a reality, they are coming, and they’re coming faster than many people appreciate.”
A Cold Departure
Topol came to San Diego in December 2006, leaving Cleveland in the middle of a blizzard. For 15 years he had overseen Cleveland Clinic’s cardiology department, which nearly tripled in size during his tenure. He also helped build a medical school and developed a 10,000-patient cardiovascular gene bank—the first of its kind.
But in 2001, he weighed in on Merck’s pain medication Vioxx, sharing his concerns that the drug might be unsafe. In 2004, Merck took Vioxx off the market; the drug increased heart attack and stroke risk. To make matters worse, the pharma giant had withheld information about the drug. Vioxx was a disaster for Merck, but Topol did not get points for being right. Some at Cleveland Clinic felt he had been too outspoken on the issue, making his position untenable. He landed in San Diego to 70-degree weather and the opportunity to remake himself.
“I ended up in the most exciting place in the world for me,” Topol says. “There’s this amazing brain trust in San Diego—not just Scripps and UCSD and Salk, but the life science industry, the information technology industry, biopharma. This cluster is the future of medicine.”
A Home in San Diego
Armed with dual appointments to Scripps Health and The Scripps Research Institute, two institutions with a history of sibling rivalry, Topol brought them together by preaching the virtues of trans-lational medicine: converting basic scientific discoveries into new therapies.
Topol helped create Scripps Translational Science Institute (STSI), bridging the gap between basic research and clinical care. One of their first projects was the Wellderly Study. Taking advantage of Scripps Health’s large patient pool, Topol’s team recruited elderly volunteers with no serious health conditions. The researchers then studied their DNA to determine which gene variations protected these “well elderly” from disease.
Meanwhile, Topol had begun building a network beyond Scripps with the J. Craig Venter Institute, SDSU, the San Diego Supercomputer Center, and others. These collaborations helped STSI gain a prestigious $20 million Clinical Translational Science Award from the NIH.
“From the start, he’s been exposing the right questions,” says Nicholas Schork, director of human biology at the Venter Institute. “What should we invest in? What technologies make sense? How can we incorporate them into health care?”
Digital Message, Digital Tools
Eric Topol believes digital technologies—genomics, smartphones, and electronic health records—will lead to “digital human beings.” Not in the dystopian sci-fi sense, but rather patients who have complete access to comprehensive health information and can make educated decisions about how to use it.
A lot of people are listening. Topol has more than 67,000 followers on Twitter (@EricTopol). He has also carved out a niche as editor-in-chief for the online news site Medscape, interviewing noted scientists and policymakers, including former Vice President Al Gore, who has become quite a fan.
“Dr. Topol is a world-class physician with a cutting-edge knowledge of digital tools and an unusual ability to communicate clearly with nonexperts,” notes Gore. “He has laid out a road map for precision, patient-centered medicine with lower costs and better outcomes and has not shied away from raising important questions about privacy and policy.”

Healthcare Goes High-Tech
Topol using a CellScope ear exam device on a 2013 episode of The Colbert Report
In 2009, Topol posed with musician Seal and USC researcher David Agus in the pages of GQ as part of an ad series called “Rock Stars of Science.” By any measure, he was at the top of his game. But there was one naysayer who thought he had more to accomplish.
“My son told me you haven’t achieved anything until you’ve been on The Colbert Report.”
Through a combination of strategic hints and old-fashioned good luck, he received an invitation in 2013 to discuss his book The Creative Destruction of Medicine on the famed Comedy Central show. Topol held his own against the notoriously aggressive Colbert persona, but his favorite part ended up on the cutting room floor.
“I got Colbert to open up his shirt and did an echocardiogram (with his smartphone). When I put the sensor on his chest, I said, ‘Stephen, it looks like you have a descending aortic aneurysm.’”
According to Topol, Colbert was taken aback for a moment before the doctor let him in on the joke. Unfortunately, despite his best efforts to obtain the video, that part of the interview may be lost to history.
Letting Patients Take the Wheel
Topol has a lot of fun with his media forays, but sees them as a tool to communicate his core message: patient empowerment. In his most recent book, The Patient Will See You Now, he takes on medical paternalism and challenges the concept that doctors always know best.
“The idea that patients should have all their information, if they want it, and have independent capabilities is not shared by a lot of doctors,” Topol says. “But as information becomes portable, this is the natural next step. We’re having a reset, where people can do diagnostics on their phone, do teleconsults, Uber doctors to their house. It’s a whole new day.”
As recently as the 1970s, physicians regularly hid cancer diagnoses from their patients for fear they “couldn’t handle the truth.” That concern persists today but in a different form: restricting access to genomic data. Topol is convinced that genetic information should not be held back.
“If people want to know if they have [the gene] ApoE4 and a higher risk for Alzheimer’s, they should know. It’s their DNA.”
Topol is not alone on this issue, but there’s an ongoing debate on whether complete genomic information might do more harm than good.
“The implications of being a gatekeeper for information and data is something we do need to be careful about,” notes Perry Nisen, CEO of the Sanford Burnham Prebys Medical Discovery Institute. “But I think we also have some obligation to help put that information into context for people.”
As the NIH implements the Precision Medicine Initiative, they are wrestling with genomic access on a grand scale—a million patients. “I think I’m with Eric that those who want the information should have access to it,” says NIH’s Francis Collins. “But it’s clear that a lot of it will be of uncertain significance, and the potential for confusion, or even scaring people, should not be neglected.”
But there may be an even more fundamental question about Topol’s vision. If you build it, will they come?
“Many people who have the time and resources to take the lead in their health care may simply choose to spend the time doing something else,” Venter’s Nicholas Schork says. “They’d prefer to rely on the health care industry and not take it on themselves.”
Crowdsourcing Solutions
When discussing disease, Topol rarely uses the word “prevention,” opting instead for “preemption.”
“Today, prevention is mostly secondary prevention—you’ve had a heart attack and you don’t want another one,” Topol says. “I’m excited about the opportunity to prevent conditions from ever occurring, to just preempt them completely. I believe we’re getting the tools to finally do that.”
At STSI, he is particularly proud of a study that sprang from the Wellderly effort. Having identified DNA regions that confer protection from heart disease, STSI researchers are now using gene transfer technology to move that DNA to heart cells to see if the protection goes with it.
And while the technology is advancing rapidly, the ultimate obstacle may be the medical profession itself. Topol notes—with more than a little anger—that few medical schools have added genomics to their curricula. Some physicians are uncomfortable with technologies they don’t fully understand; others avoid these tests because the turnaround times are too long.
“For many drugs, there’s genomic data saying there could be a fatal side effect or the drug will be ineffective,” Topol says. “We don’t use these enough because of this pervasive resistance.”
Frustrated that this potential is slow in being realized, Topol sees solutions in emerging digital technologies and consumers willing to embrace them.
“Most of the things that are wrong with medicine already have a fix,” he explains. “We just need to ante up with a whole different approach. For the people who want to be engaged, the technology is coming quickly to make that happen.”

Healthcare Goes High-Tech
Dr. Eric Topol | Photo by Robert Benson | Hair & Makeup by Melissa Graaff














